AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
Back to Blog
Amniotic fluid embolism treatment2/27/2023  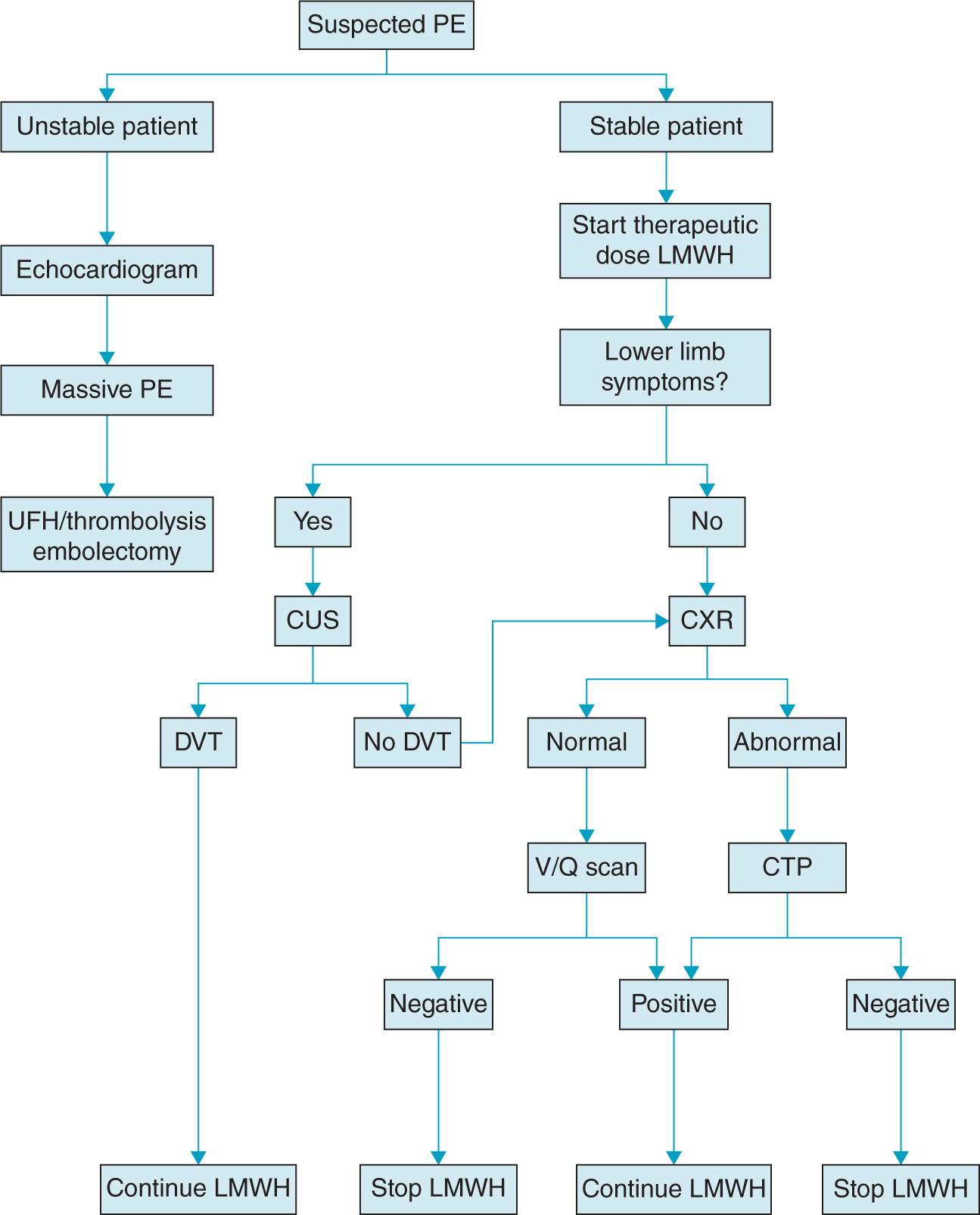
Sodium bicarbonate, calcium, furosemide, albuterol were used to treat rising potassium. ABGs demonstrated profound metabolic and respiratory acidosis (pH 104, HCO 3 = 15, BE = -21) and hyperkalemia. Spontaneous cardiac activity was never noted on TEE throughout the resuscitation and PEA continued.Īrterial blood gases (ABG) and coagulation studies also deteriorated throughout the resuscitation (Table 1). Transesophageal echocardiography (TEE) was performed. Chest compressions were monitored to be high quality by the mean arterial pressure on the arterial line and capnography. Both central IV and arterial access were obtained. In addition to epinephrine and vasopressin per ACLS protocol, intravenous (IV) heparin was initiated to treat possible pulmonary embolism. The differential diagnosis included allergic reaction, pulmonary embolism, and amniotic fluid embolism. Treatment with epinephrine and atropine briefly improved hemodynamics, but Pulse less Electrical Activity (PEA) developed within 30 seconds.Īdvanced Cardiac Life Support (ACLS) was initiated. Approximately 2 minutes after amniotomy, ETCO 2 dropped (34 to 11) followed quickly by hypotension (60/40), oxygen desaturation and bradycardia. Rupture of amniotic membranes was noted and an expected amount of amniotic fluid was evacuated using suction (65 mmHg). Osmotic dilators were removed, further cervical dilation was achieved with Pratt dilators, and a 14 mm cannula inserted for evacuation via suction. In the operating room, general anesthesia induction and intubation were uneventful. All laboratory values were within normal limits and an EKG from one month prior was unremarkable. On the day of dilation and evacuation, preoperative laboratory tests were drawn (Table 1). Her procedure was scheduled the day following dilator placement (two days following diagnosis of fetal demise). As the patient elected to undergo surgical treatment, osmotic cervical dilators were placed the next day. This pregnancy had reached 24 weeks gestation by 14 week ultrasound however, routine 24 week gestation ultrasound demonstrated a fetal demise measuring 19 weeks by fetal biometry with a normal amniotic fluid volume. She had one hospitalization at 21 weeks gestation for hypertensive urgency that was treated with intravenous medications and transitioned to oral therapy prior to discharge. Obstetrical history included a classical cesarean section in her first pregnancy secondary to pre-eclampsia and an uncomplicated, term repeat cesarean delivery for her second pregnancy. The patient’s medical history included hypertension, diet-controlled type II diabetes mellitus, tobacco and marijuana abuse, and obesity (BMI 30.4 cm²/kg). 
0 Comments
Read More
Leave a Reply. |
 RSS Feed
RSS Feed